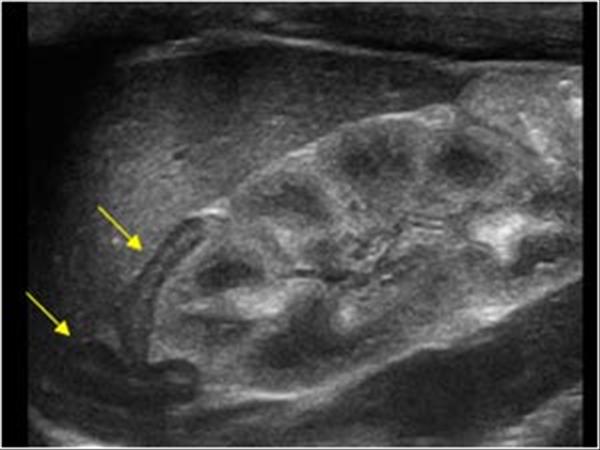
Gray-scale imaging may show a marbled, reticulated pattern when edema collects in the subcutaneous fat. This is very different from the typical biphasic (above and below the baseline) pattern seen with venous congestion. Blood flow in the fistula will only be in one direction toward the venous or lower-pressure side without reversal of flow. 
The waveforms identified from both the arterial and venous sides of an AVF will show an arterialized pattern with a low-resistance (high-diastolic) component. Although blood flow patterns seen with both venous congestion and AVF will demonstrate increased pulsatility, there are major differences. Pulsatile venous waveforms from venous congestion are frequently mistaken for signals associated with arteriovenous fistula (AVF). This does not occur on the arterial side. Another distinguishing characteristic is the change in venous flow that occurs with the Valsalva maneuver. Other clues to the nature of the flow abnormality are the direction of flow and the communications with the superficial veins. On close inspection, the phases of the venous pattern are less periodic than the typical triphasic waveforms found in the arterial system. Comparison of the arterial and venous flow patterns is key to distinguishing pulsatile venous signals from arterial flow. Pulsatility in the venous system may resemble arterial pulsations because of the bidirectional pattern of blood flow. These changes result in increased pulsatility in the peripheral vein waveforms. 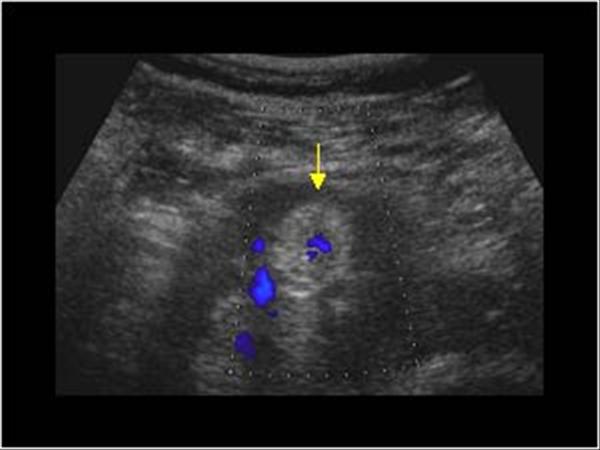
As noted in Chapter 1, causes of increased venous pressure such as heart failure or tricuspid insufficiency lead to increased transmission of cardiac phasic changes in pressure and blood flow to the peripheral veins of the upper and lower limbs. In right-sided heart failure, the waveforms are usually more pulsatile and typically bidirectional, with components seen above and below the baseline ( Fig. We expect to see phasic, nonpulsatile waveforms in the normal lower extremity veins. There is a change in venous flow patterns in cases of heart failure. These problems result in leg swelling and soft tissue edema. Causes of increased hydrostatic pressure within the venous system include heart failure (HF venous congestion), fluid overload, deep vein thrombosis (DVT), venous compression, and other causes of venous obstruction. Lower extremity edema is a common cause of limb swelling and is associated with either elevated venous pressures or lymphatic obstruction (lymphedema), or both.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
